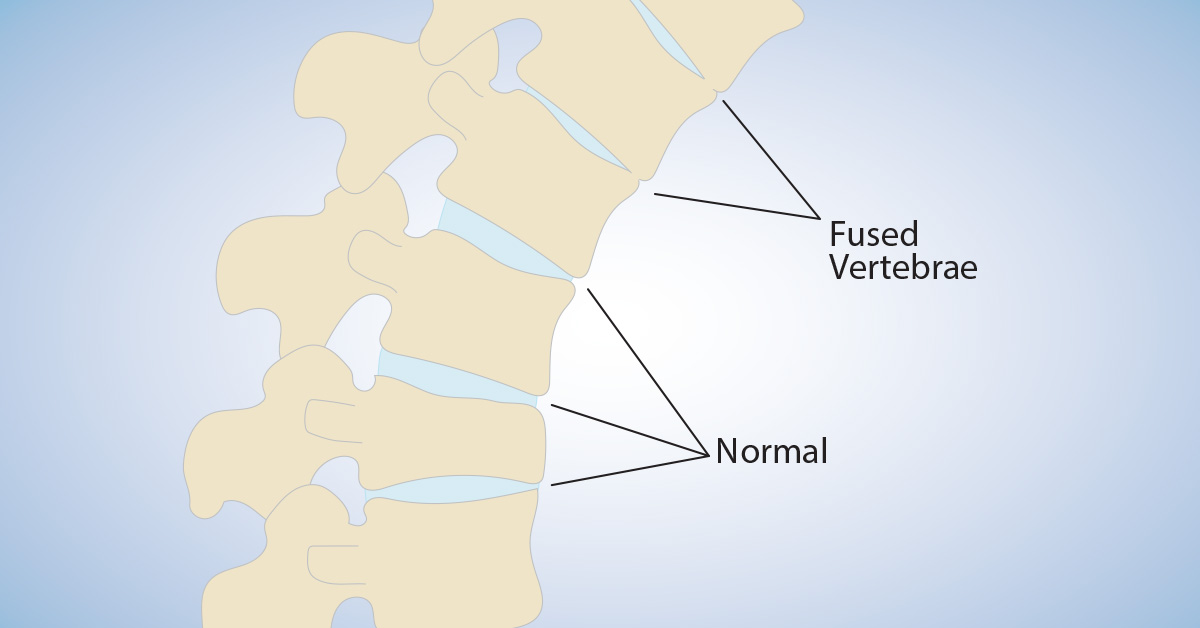
Ankylosing spondylitis is a disease of the vertebra. It is characterized by inflammation of the spinal column leading to fusion of the individual vertebra to each other.
In this article, we shall briefly look at this condition and how it affects the patient.
What is Ankylosing Spondylitis?
Ankylosing spondylitis is an inflammatory condition of the spinal column. This inflammation leads to fusion of the vertebra to each other, causing the spine to become bent in a forward direction. The condition is more common in men and usually starts in early adulthood.
What Causes Ankylosing Spondylitis?
Research has shown that ankylosing spondylitis is an inherited condition that has a genetic basis. In particular, a gene called HLA B27 is responsible for the development of this condition.
What Are the Symptoms?
In the early stages there may not be many symptoms that can aid diagnosis of the condition. However, as the condition progresses, individuals may begin to experience pain and stiffness in the lower back and hips. Typically, the condition affects the lower back and hips but over time can involve the entire spine. Other areas that may be involved are the shoulder joint, cartilage in the front of the chest and the cartilage around the heel.
How is a Condition Diagnosed?
A diagnosis of ankylosing spondylitis is made with the help of an X-ray of the spine. Typically, the appearance has been described as 'bamboo spine.' The spinal column is arranged like a stick of bamboo.
During clinical examination, the doctor may attempt to elicit different spinal movements to determine the degree of loss of flexibility associated with ankylosing spondylitis. Other tests may include lung capacity studies. There are no specific laboratory tests that can help diagnose ankylosing spondylitis, though genetic studies have been conducted to determine the presence or absence of the specific gene previously mentioned. It must be kept in mind that the presence of the HLA B27 gene does not necessarily mean that the person has ankylosing spondylitis.
In certain cases, an MRI of the spine can be useful in diagnosis of the condition.
Treatment
The aim of treatment is to reduce pain and restore mobility. Lifestyle changes such as stopping smoking and weight reduction are recommended. Non-steroidal anti-inflammatory drugs (painkillers) are useful in the early stages. In the event that these drugs do not help reduce pain, more specific agents such as tumor necrosis factor blockers (TNF blockers) may be utilized. These drugs are only administered by an experienced rheumatologist and are not available over-the-counter.
Physiotherapy is another avenue that is often pursued in the management of this condition. Range of motion exercises and stretches are advised to patients with the aim of maintaining normal posture and preventing further deterioration.
Advanced cases that do not respond to medical therapy or physiotherapy may require surgical correction.
