You may be a candidate for Endoscopic Foraminotomy
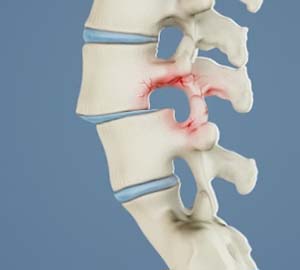
Spondylolisthesis
Over the years, we ask a lot of our spine. Through a person’s lifetime, this interdependent and essential structure helps support the weight of the upper body, protects the spinal cord, and facilitates movement. Eventually, the strain that results from these responsibilities begins to have consequences. Intervertebral discs lose water content, and the structural quality of the vertebral column starts to deteriorate. Besides the general wear and tear that occurs as we age, spinal injuries can happen at any point in an individual’s life. Traumatic injuries often happen suddenly and may disrupt proper functioning. All of these factors generally contribute to the development of harmful spinal complications.
The term “spondylolisthesis” refers to one such condition that occurs when a vertebra in the spine slips forward and slides over the bone below it. Although spondylolisthesis most commonly occurs in the lumbar (lower back) region, this condition may develop in the cervical (neck) and thoracic (middle back) areas of the spine as well. Oftentimes, spondylolisthesis will place tremendous pressure on the spinal cord and surrounding nerves, which in turn leads to intense pain and discomfort. Some patients may experience no symptoms or delayed symptoms that surface well after the original post-vertebral slip. Others will notice immediate discomfort as soon as the vertebra shifts. If spondylolisthesis is causing pain and other debilitating symptoms, there are many safe, evidence-based methods to address this condition and encourage restoration to a patient’s quality of life.
Causes
Spondylolisthesis most often ensues after a fracture, but there are many causes that can contribute to this disorder, including:
- Congenital defective joints, genetics, and family history
- Sudden injuries or traumas which commonly occur as the result of manual labor, high-impact sports, hard falls, or unexpected accidents
- Overuse of the affected joint
- Frequent, improper movements or lifting
- Aging and general wear and tear associated with the aging process
- Infection
- Arthritis
- Conditions, such as degenerative disc disease, that affect the behavior of intervertebral discs
- Obesity
- Lack of exercise
- Malnutrition
- Smoking and the excessive consumption of alcohol
The above causes play a central role in many back-related conditions besides spondylolisthesis. For this reason, it is important to seek medical attention as soon as you realize you are experiencing a spine complication. Receiving an accurate, prompt diagnosis will better your chances of attaining the most optimal treatment possible.
Symptoms
The symptoms of spondylolisthesis vary widely depending on the location and severity of the displaced vertebrae. However, some of the most common indicators of spondylolisthesis are:
- Pain or numbness in the buttocks or legs, if spondylolisthesis has occurred in the lower back region
- Weakness in lower back and affected extremities
- Difficulty walking and performing other everyday tasks
- Low back pain that worsens when a patient twists or bends over
- Sciatica
Some patients encountering spondylolisthesis may have no symptoms at all. The problems associated with this condition usually only arise when the problematic vertebrae begin to compress one or more nearby nerves.
Our Microspine & Minimally Invasive Treatment Approach
If left untreated, spondylolisthesis can lead to an array of related spine complications and may begin to significantly impact your health and well-being. By proactively addressing spondylolisthesis, you can take control of your condition and lessen or even eliminate inhibiting symptoms. From diagnosis to recovery, Dr. T is committed to helping you achieve a pain-free life, so that you can return to the activities you love faster.
The first step toward finding relief from spondylolisthesis is to schedule a consultation at one of our conveniently located spine clinics. During this initial visit, Dr. T will attentively evaluate your medical history, physical state, and symptoms. To diagnose spondylolisthesis and determine its severity, a C.T. scan, MRI, or X-ray may be required. This also helps us to rule out other, similar conditions.
Whenever possible, we encourage patients to consider conservative, non-invasive treatments before looking into surgical intervention. Spondylolisthesis can be responsive to non-surgical treatments, such as:
- Physical Therapy: When combatting spondylolisthesis, the primary goals of physical therapy are to strengthen the core muscles which support the spine. In addition, physical therapy may help patients improve their flexibility and lose excess pounds. Being overweight or obese can worsen spondylolisthesis by placing immense pressure on the spine and leading to additional difficulties within the back region.
- Medication: Anti-inflammatory and pain-relieving medications can reduce the amount of discomfort caused by spondylolisthesis.
- Additional Modifications: For some patients, assistive devices, heating and cooling therapies, a limited period of rest, or other alternative treatments may be recommended. Every component of care depends upon the patient’s unique case of spondylolisthesis, as well as their goals and lifestyle.
In cases where spondylolisthesis is causing the vertebrae to continually move or in situations where the spine requires stabilization, surgical intervention may be necessary right away.
Some patients may need only Microspine endoscopic decompression utilizing extremely small incisions and tiny cameras without fusion, whereas others may need Minimally invasive spine fusion (MIS-TLIF) which Dr. T can customize and tailor for each patient as there is no “one size fits all” in medicine.
The Microspine & minimally invasive surgeries available that we offer generally lead to:
- Shortened recovery times that enable patients to return to their daily routines and lives more quickly
- Less post-operative pain than what is statistically linked to traditional open surgeries
- A minimal risk of scarring or trauma to surrounding tissues
- Significantly reduced blood loss than what is typically experienced in open back surgery
We look forward to helping you feel better, faster! CONTACT US
